- Home
- PA Resources
- Clinical INsights
IAPA - Clinical INsights
Teen pregnancy outcomes can improve with specialty collaboration Sweta Gupta, MD – Pediatric Hematologist Magdalena Lewandowska, MD – Adult Hematologist Innovative Hematology, Inc. and Indiana Hemophilia & Thrombosis Center Adolescent pregnancy continues to present challenges to healthcare teams nationwide. The healthcare community at large needs to identify ways to help improve outcomes for both adolescent mothers and their babies. JAMA recently published a study suggesting that teen pregnancy may be an identifiable marker for premature mortality in early adulthood. 1 The study, based in Ontario, Canada, analyzed pregnancy outcomes in 2.2 million adolescent girls who were 12 years old between April 1991 and March 2021. After accounting for pre-existing health conditions and income and education disparities, adolescents who carried pregnancies to term were found to be more than twice as likely to suffer premature death later in life. 1 The challenges of adolescent pregnancy The average onset of menarche is 12.4 years 2 —typically occurring between ages 10 and 16 years when these adolescents are still under the care of pediatric or family practice providers. The American College of Obstetricians and Gynecologists (ACOG) recommends teens make their first reproductive health visit between the ages of 13 and 15. 3 In many cases of adolescent pregnancy—often considered pregnancy between the ages of 13 and 19—this first gynecological exam is prompted by the pregnancy. Denial about their ability to become pregnant can lead to a later diagnosis and potentially increased health risks for the teen mother and her baby. 4 For this reason, early detection of pregnancy is key to decreasing perinatal risks. If an adolescent presents with amenorrhea, vomiting, nausea, breast tenderness, fatigue, weight gain, dizziness, abdominal pain, irregular menstruation, and any other symptoms typically associated with pregnancy, the possibility of pregnancy should be considered. Pediatric providers are not typically trained to manage or counsel a pediatric patient through pregnancy making it even more important to connect with an obstetrician experienced in adolescent reproductive medicine. The importance of co-management All cases of adolescent pregnancy should be treated as high risk. 5 Special consideration should also be given to whether the pregnant teen has a personal or family history of bleeding or thrombosis. There is an average of 16 years between the onset of bleeding symptoms and the diagnosis of a bleeding disorder in women and girls. 6 It is therefore possible that a pregnant adolescent with a blood disorder could be diagnosed at their first OB/GYN appointment. Studies supporting treatment guidance for pregnant adolescents with blood disorders are limited at best, underscoring the importance of collaboration between pediatric hematology, adult hematology and OB/GYN practitioners. For example, compared to the general population, adolescent girls are at higher risk for venous thromboembolism (VTE). Their VTE risk peaks between the ages of 15 and 18 and often increases further into their pregnancy. Because no studies exist related to VTE risk in pregnant adolescents, providers must rely on recommendations for pregnant adults to guide care. 7 This lack of pediatric pregnancy data can be the case for many blood disorders—not just thrombosis—and impacts approaches to management. What’s more, the pregnant patient in these scenarios is a child, making co-management of their care between adult and pediatric hematology with close communication with OB/GYN is immensely valuable. Different risks must be considered depending on the patient’s specific blood disorder, including:
Pregnant adolescents and their newborns are also at higher risk of bleeding complications compared to the general population. For example, the crucial decision between cesarian versus vaginal delivery should be a decision made as a team considering the pregnant adolescent’s underlying hematologic disorder. The decision is largely influenced by the risk of postpartum hemorrhage for the mother and intracranial hemorrhage for the newborn. 8 In cases of pregnant adolescents with sickle cell disease (SCD) who present to the ER or delivery room, the delivering provider should immediately connect with hematology, as management can be complex. Pregnancy increases the demand for red cell mass. Blood transfusions or exchange transfusions may be necessary due to the already low hemoglobin in patients with SCD. Some experts even recommend transfusing to a goal hemoglobin of 10 g/dL prior to cesarean delivery. These recommendations are not universal and there is considerable nuance, hence the need to consult with an expert in sickle cell disease. 9 An advanced model of coordinated care Healthcare systems should evaluate their approaches to adolescent reproductive health and whether appropriate training and specialties are in place to properly manage both a pregnant adolescent’s health and their chronic condition. Innovative Hematology and IHTC’s GO+ Clinic is a model of provider comanagement of blood/bleeding disorders in pregnancy. GO+ Clinic is the only specialty clinic of its kind in Indiana, providing comprehensive, coordinated care for menstrual and gynecological health. At GO+ Clinic, pregnant adolescents with various hematological conditions are comanaged by their pediatric hematologist, an adolescent medicine physician and/or gynecologist, and an adult hematologist, depending on the complexities their blood disorders bring to their pregnancies. Hematological conditions may include any of the below:
The team is also ready to address the psychosocial challenges of this otherwise lost population of young moms. For example, a clinical psychology and social work team is available to provide social support, help address patients’ delayed or neglected educational goals, and ensure they pursue antenatal care. In addition to the importance of a stable family life and peer and school support, the JAMA study also cites the importance of “… open communication with adult mentors or parents about contraception use, free access to contraception, and female empowerment to abstain from unwanted or unplanned intercourse.” 1 Medical caregivers should evaluate their readiness to educate young patients in the case of unintended pregnancy. Awareness of their options and available resources can have a positive impact on outcomes.However, first and foremost, pediatric providers should be trained in counseling young girls against early pregnancy to prevent it altogether. Proactive counseling about reproductive health and the consequences of unplanned pregnancy can play a role in reducing these cases from the start. Drs. Sweta Gupta and Magdalena Lewandowska are pediatric and adult hematologists, respectively, and part of the care team at Innovative Hematology, Inc. (IHI) in Indianapolis. IHI treats blood disorders—from common to rare—every day, and is a certified medical home recognized for excellence in comprehensive patient-centered health care. The care providers of IHI treat sickle cell disease, thalassemia, HHT and nutritional anemias, as well as many other blood disorders. IHI is home to the Indiana Hemophilia and Thrombosis Center (also known as the IHTC, a 501(c)3), the only federally recognized comprehensive hemophilia treatment center in Indiana and one of the nation’s top hemophilia treatment centers. The IHTC treats rare bleeding disorders such as hemophilia, von Willebrand disease, other rare factor deficiencies, and clotting conditions. The organization is both nationally and internationally distinguished as a Center of Excellence for leadership in blood disorder patient care, education, and research. Learn more at www.innovativehematology.org 1. Ray JG, Fu L, Austin PC, et al. Teen Pregnancy and Risk of Premature Mortality. JAMA Netw Open. 2024;7(3):e241833. doi:10.1001/jamanetworkopen.2024.1833 2. Lacroix AE, Gondal H, Shumway KR, Langaker MD. Physiology, Menarche. In: StatPearls. Treasure Island (FL): StatPearls Publishing; March 11, 2023. 3. The initial reproductive health visit. ACOG Committee Opinion No. 811. American College of Obstetricians and Gynecologists. Obstet Gynecol 2020;136:e70–80. 4. Teenage Pregnancy. MedlinePlus. Updated April 30, 2018. Accessed April 22, 2024. https://medlineplus.gov/teenagepregnancy.html#:~:text=Teen%20pregnancies%20carry%20extra%20health,and%20a%20low%20bi rth%20weight 5. Diabelková J, Rimárová K, Dorko E, Urdzík P, Houžvičková A, Argalášová Ľ. Adolescent Pregnancy Outcomes and Risk Factors. Int J Environ Res Public Health. 2023;20(5):4113. Published 2023 Feb 25. doi:10.3390/ijerph20054113 6. Data and Statistics on von Willebrand Disease. Centers for Disease Control and Prevention. Reviewed July 7, 2023. Accessed April 22, 2024. https://www.cdc.gov/ncbddd/vwd/data.html#:~:text=There%20was%20an%20average%20of,surgery%2C%20injury%2C%20and%2 0delivery 7. Srivaths LV. Hematology in the Adolescent Female. Springer Cham; 2020:311–312. 8. Niu B, Duffett L, El-Chaâr D, Tinmouth A, Wang TF, Khalife R. Bleeding disorders and postpartum hemorrhage by mode of delivery: a retrospective cohort study. Res Pract Thromb Haemost. 2023;7(4):100166. Published 2023 Apr 26. doi:10.1016/j.rpth.2023.100166 9. James AH, Strouse JJ. How I treat sickle cell disease in pregnancy. Blood. 2024;143(9):769-776. doi:10.1182/blood.2023020728 THE NEW AGENCY FOR HEALTHCARE RESEARCH AND QUALITY (AHRQ) SAFETY PROGRAM FOR TELEMEDICINE: IMPROVING ANTIBIOTIC USE The new Agency for Healthcare Research and Quality (AHRQ) Safety Program for Telemedicine: Improving Antibiotic Use. This is a no-cost program that seeks to promote appropriate antibiotic use while maintaining patient satisfaction and reducing potential side effects in patients seen via telemedicine. AHRQ is currently recruiting primary and urgent care facilities to participate in the program. This program, beginning in June 2024, consists of brief educational presentations about best practices to optimize antibiotic prescribing in the telemedicine environment. Participants will have access to technical assistance, coaching, webinars, and practical tools to implement improvements in their practice. The program is offering credit via the American Medical Association (AMA), American Nurses Credentialing Center (ANCC), American Board of Internal Medicine (ABIM) Maintenance of Certification (MOC), American Academy of Physician Associates (AAPA), and Interprofessional Continuing Education (IPCE) to participants at no charge. WORKING WITH YOUTH AND THEIR FAMILIES TO PROMOTE INDEPENDENT HEALTH SKILLS AND COMMUNICATION By Brittany Savage, Nurse Practitioner, Indiana Hemophilia & Thrombosis Center (IHTC) Do you remember the first time you entered a doctor’s office without your parents by your side, or when you called a pharmacy for the first time for your own prescription? Young patients often have a caregiver who makes their appointments and speaks for them during healthcare visits. Without partnering with their parent/caregivers and healthcare providers to work toward self-management, they can feel lost as they become young adults and take the first step into managing their own health matters. Read more ...Transition for Families Transitioning from childhood to adulthood can be challenging for everyone in the family. Healthcare management is no exception. As children get older, they need to learn to manage their healthcare while parents and caregivers learn how to step into a new supportive role. This transition is different for each family. Pediatric care teams should start a discussion with families well before the child transfers to adult care. Together, they can plan for age-appropriate opportunities for the child to care for their own medical needs. A Provider’s Role Transition means to change from one way of doing things to a new way. As young patients grow, they will learn new skills and information to take care of themselves. Transfer of care is when a patient must transfer−or move−care to an adult doctor. This is part of the transition process. Providers can assist throughout the transition process by giving pediatric patients learning opportunities to be more independent and confident, such as: Address the Patient – Some providers fall into the pattern of talking to the parents or guardians rather than to the patient. Speaking to the patient directly and giving them the opportunity to ask or answer questions gives the patient a voice. Phone Calls - If the patient has not spoken with triage or made appointments on their own, have them begin listening to their parents or caregivers when they call the office. They can quickly learn how to make their own calls and possibly even write a phone script for future use. Pharmacy – Encourage the patient to take regular medications without prompting and remember to take their medications on time. Appointments - Mark a calendar with important health reminders and appointments. Assess Healthcare Self-Management Milestones – Since transition looks different for each patient, discuss what different milestones look like for them and how the care team is there to support them. Don’t forget that parents/caregivers are going through their own transition during this time as well. It can be difficult to learn to step back from caretaking duties while maintaining oversight. Supporting parents during this time is important. The best way to ensure a patient is prepared for their transition to adult care is to collaborate with the family as a team. Encouragement from the parents, caregivers and healthcare team will lead to success. Brittany Savage is a nurse practitioner at the Indiana Hemophilia & Thrombosis Center (IHTC) in Indianapolis. She dedicates much of her career to teaching families of young children with chronic bleeding disorders how to develop skills and knowledge to eventually self-manage their healthcare. Transition for FamiliesTransitioning from childhood to adulthood can be challenging for everyone in the family. Healthcare management is no exception. As children get older, they need to learn to manage their healthcare while parents and caregivers learn how to step into a new supportive role. This transition is different for each family. Pediatric care teams should start a discussion with families well before the child transfers to adult care. Together, they can plan for age-appropriate opportunities for the child to care for their own medical needs. A Provider’s RoleTransition means to change from one way of doing things to a new way. As young patients grow, they will learn new skills and information to take care of themselves. Transfer of care is when a patient must transfer−or move−care to an adult doctor. This is part of the transition process. Providers can assist throughout the transition process by giving pediatric patients learning opportunities to be more independent and confident, such as: Address the Patient – Some providers fall into the pattern of talking to the parents or guardians rather than to the patient. Speaking to the patient directly and giving them the opportunity to ask or answer questions gives the patient a voice. Phone Calls - If the patient has not spoken with triage or made appointments on their own, have them begin listening to their parents or caregivers when they call the office. They can quickly learn how to make their own calls and possibly even write a phone script for future use. Pharmacy – Encourage the patient to take regular medications without prompting and remember to take their medications on time. Appointments - Mark a calendar with important health reminders and appointments. Assess Healthcare Self-Management Milestones – Since transition looks different for each patient, discuss what different milestones look like for them and how the care team is there to support them. Don’t forget that parents/caregivers are going through their own transition during this time as well. It can be difficult to learn to step back from caretaking duties while maintaining oversight. Supporting parents during this time is important. The best way to ensure a patient is prepared for their transition to adult care is to collaborate with the family as a team. Encouragement from the parents, caregivers and healthcare team will lead to success. Brittany Savage is a nurse practitioner at the Indiana Hemophilia & Thrombosis Center (IHTC) in Indianapolis. She dedicates much of her career to teaching families of young children with chronic bleeding disorders how to develop skills and knowledge to eventually self-manage their healthcare. |
How I Overcame Burnout by Moving to an Employer Health Center to Focus on Outcomes-Based CareBy Brooke Curry, Physician Assistant, Marathon Health I recently celebrated my seventh anniversary working as a physician assistant within an employer-sponsored healthcare model that prioritizes positive outcomes. And while I truly love my job and the work-life balance it affords me, things weren't always this way. Not even close. Before joining Marathon Health as a physician assistant, I spent years grinding away in a perpetually busy, one-provider clinic. I’d typically see 25 to 30 patients each day. Appointments lasted 15 minutes at best. In my industry, we all went to school because we want to help people live healthier lives — and my heart was certainly in the right place — but time simply wasn't on my side. I constantly felt like I’d take one step forward, and then three steps back. Something new would always pop up during a visit, or I’d want to talk to a patient about a different approach. It left me feeling burnt out and unsatisfied in my role. A New Approach to Primary CareEverything changed after I received a flyer in the mail inviting me to a dinner in Indianapolis. It mentioned there'd be a casual discussion about this new revolutionary way of providing healthcare. Jeff Wells, MD, and CEO of Marathon Health, led the discussion. Anybody who has ever met Jeff knows he's extremely passionate about healthcare. You can genuinely tell he believes everything he says. It didn’t feel like a sales pitch. He mentioned how we would have more time with our patients. Time to connect and get to know them on a personal level. Time to focus on preventing chronic disease. He said, “We'll allow you to make the decision on what you feel is best for your patient.” It all sounded amazing. It was exactly why I went to PA school in the first place. A Typical Day in an Employer Health CenterNow, I run the Marathon Health Network primary care clinic in Plainfield. We have two nurses, an RN and LPN, on our main crew, and a health coach and behavioral health specialist who visit a few days per week. Our health center has a different kind of vibe. It’s not slow-paced, but you can tell the care team feels more relaxed, versus running around because they’re already three patients behind. It's a kind of Zen-like feeling around here, and our patients notice it as well. The minimum visit with my chronic patients lasts 30 minutes. I have the freedom to add on as much time as I want. And since we're not billing insurance, I don't have to justify the fact that I feel like one patient needs 60 minutes, while another only needs 20 minutes. It's common for my patients to have high blood pressure, diabetes, hyperlipidemia, depression, and anxiety. We also provide preventive health screenings, including mammograms and pap smears. I could be doing only physicals one day and removing a foreign object from someone’s finger the next day. I have plenty of time to not only meet with my patients for whatever they need, but if they have an acute complaint they also want to discuss during the appointment, there's time for that, too. Embracing Work-Life Balance My work-life balance has drastically improved since transitioning to an employer health center. I’m extremely passionate about healthcare, but it doesn’t define me. I also have three kids and this whole other life outside of work. I don't think my previous employers even knew I was a mom. Now, I feel like my employer cares about me as an individual. They understand I have a life. We don’t work weekends or evening hours. I'm done at four each day, so I have time to pick up my kids from school, and I'm able to get them to their sporting events. The model works because it gives me time to be better at my job, and helps me mentally by allowing me time with my family. I arrive refreshed and ready to serve my patients. And I really love my patients. I've worked in the same health center and treated the same patients for seven years. That’s a huge chunk of time to be involved in somebody's life. I truly look forward to seeing them, and it makes me happy to show up to work every day. Ultimately, my job allows me to be present for my patients, and then once their needs are met and my shift ends, I'm ready to start my second job, which is being a wife and a mother. Bio: Brooke Curry has been a Physician Assistant for seven years at Marathon Health, an employer healthcare model that has worksite locations in 43 states, including Indiana; 7 Network locations in and around Indianapolis; and virtual care nationwide. Brooke completed her PA degree in Billings, Montana, in 2008 when she began providing primary care to the underserved and homeless population. She has also worked in primary care in North Carolina. Today, she resides in a rural town in central Indiana with her husband, three children and two dogs. |
Connect your patients with rare disease resources
By Kimber Blackwell, MPAS, PA-C
Indiana Hemophilia & Thrombosis Center
You had a 1 in 365 chance of having your exact birthday, assuming it’s not on Leap Day. If your birthday is on Leap Day—the rarest day on the calendar—your odds were 1 in 1,461.
The rarity of Leap Day is exactly why a movement on rare diseases—Rare Disease Day—selected the last day of February to raise global awareness about uncommon conditions. Rare Disease Day is celebrated every three years on February 28, and on February 29 every four years.
According to rarediseaseday.org, a disease is considered rare if it affects less than 1 in 2,000 people.
We all know that unlike rare conditions, common disorders tend to have a straightforward path to diagnosis. If a patient has allergies, for example, symptoms are usually obvious and prompt a visit to a primary care provider. Testing for common allergies tends to be very accessible, typically leading to a timely and accurate diagnosis and effective treatment plan.
But for people living with a rare condition, this isn’t always the case.
Symptoms don’t always show the whole picture in rare diseases, even after testing and analysis. Well-meaning and seasoned primary care providers and subspecialists don’t always have the proper expertise to correctly identify or treat rare conditions. The limited amount of available scientific knowledge can be a roadblock, and waiting can be a scary and expensive road for patients looking for answers and relief.
I’m a PA in hematology, and my clinic sees patients from all over Indiana and across the globe living with rare—and sometimes ultra-rare—bleeding and blood conditions. Patients with Hemophilia, PAI-1, Plasminogen Deficiency, Hereditary Hemorrhagic Telangiectasia (HHT), G6PD, Sickle Cell Disease and Thalassemia are diagnosed and treated at our center. A common theme we hear is the stress their conditions have brought to their lives, including the uncertainty and complicated journey that eventually led them to our office. We also commonly see their relief after accessing necessary and life-saving treatments.
Relief for people living with a rare disease should not be far from reach. These patients often need more than clinical treatment, they need a community of peers and resources to support them in all aspects of life beyond the clinical setting.
Please remember that if you encounter a patient with a rare disease, that many rare conditions are supported by advocacy groups and can be found through websites like rarediseasesnetwork.org. The National Institutes of Health is also a valuable resource. Visit rarediseases.info.nih.gov for extensive information on rare diseases, including a directory of advocacy organizations.
Encourage your patients to remain steadfast as they search for answers for their or their loved one’s health concerns. Your encouragement and help in connecting them with resources could significantly and positively affect their outcomes.
Kimber Blackwell MPAS, PA-C, is a physician assistant at the Indiana Hemophilia & Thrombosis Center in Indianapolis. In addition to working with bleeding and blood disorder patients—particularly with Sickle Cell Disease—Kimber participates in education efforts for U.S. hemophilia treatment center providers and works extensively on national bleeding disorder advocacy initiatives.
HHT: Underdiagnosed, but what is it?
By: Magdalena Lewandowska, MD
Adult Hematologist-Oncologist
Indiana Hemophilia & Thrombosis Center
About 1 in 5,000 people are affected by Hereditary Hemorrhagic Telangiectasia (HHT), a rare and underdiagnosed vascular disorder. Advanced Practice Practitioners (APPs) are in a position to be able to help identify patients with HHT and direct them to receive disease-specific care, which may be lifesaving.
HHT, also known as Osler-Weber-Rendu Syndrome, is an autosomal dominant genetic disorder that results in abnormal formation of blood vessels, leading to symptoms such as:
- Nosebleeds
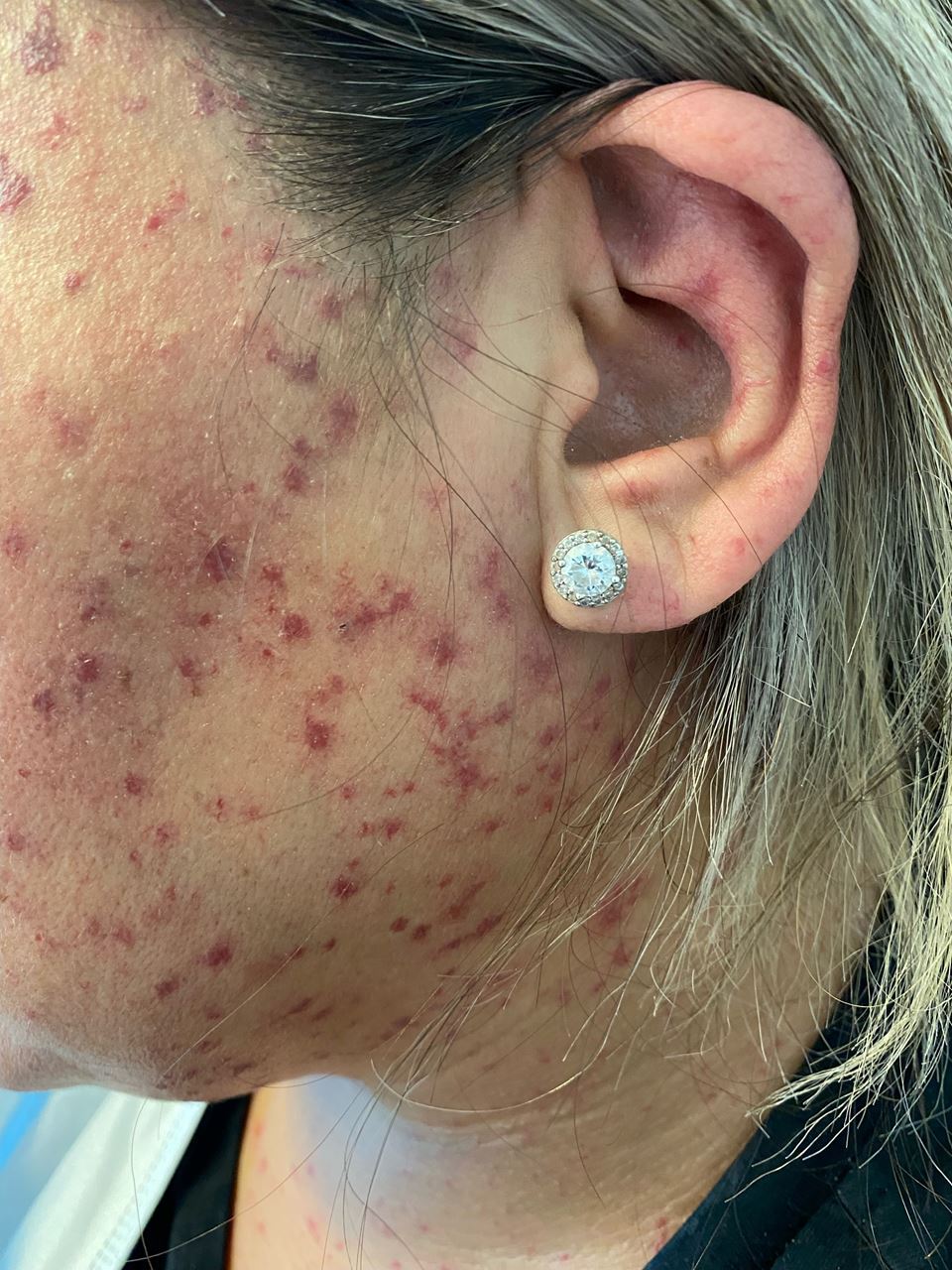
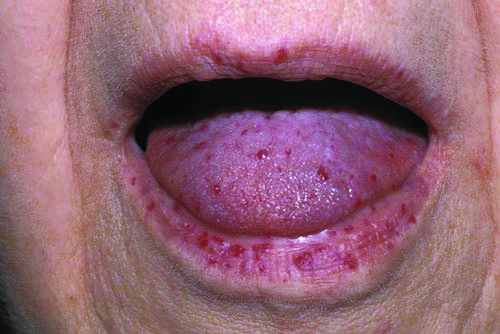
- Skin and oral telangiectasia (visible red spots)
- Arteriovenous malformations (AVMs) in various organs, such as lungs, brain, and liver
- Iron deficiency anemia
Many patients experience delay in diagnosis and do not receive appropriate testing or treatment in a timely manner. Left untreated, AVMs caused by HHT may result in bleeding, stroke, brain abscesses, heart failure, and even death.
While there is not yet a cure for HHT, early diagnosis and screening tests can improve outcomes. 90% of people with the disease do not currently know they have it because of a lack of awareness. Globally, an estimated 1.4 million people are living with HHT, which presents equally in persons of all genders, races, and ethnicities.
David L. is an Indianapolis-area resident living with the condition, and he was first referred to seek treatment in Chicago. His heavy daily nosebleeds and lengthy travel for care were burdens on work and family life, until he learned about the Indiana Hemophilia and Thrombosis Center (IHTC) in Indianapolis, which is home to the state’s only HHT Clinic.
The global patient advocacy group, CureHHT, has designated IHTC an HHT-HTC Treatment Center through a program funded by the Centers for Disease Control (CDC). The program has helped identify 150 patients living with HHT in the state of Indiana. The HHT-HTC Treatment Center at IHTC takes a multidisciplinary approach to screening, diagnosis, and management of the disease. Led by adult and pediatric hematologists, an integrated team of specialists provides lifelong, comprehensive care for patients with HHT.
HHT-related symptoms vary between individuals, and patients may need referrals to otolaryngology, interventional radiology, pulmonology, gastroenterology, neurosurgery, cardiology, or other specialists. IHTC brings patients access to various subspecialists with HHT specific expertise. In addition, a multidisciplinary team is available to address the whole-life impact HHT may have on patients with HHT, including physical therapists, dietitians, dental hygienists, social workers, and academic/career counselors.
Patients like David are treated for their condition locally, and with the burdens of travel off their plates they can focus on other aspects of life with the help of IHTC’s multidisciplinary team. In fact, now that his nosebleeds are under control and he is able to focus on his career, David is finally pursuing his dream of becoming a licensed educator and is able to spend more time with his son.
HHT is a hereditary disease, and IHTC provides genetic counseling, testing, and screening for patients’ at-risk relatives. The story of Carmel, Ind., residents Case and Eve is an excellent testament to the impact that may arise from testing at-risk family members. Joseph was diagnosed with HHT after a serious health emergency, which led to the diagnosis of his children through genetic testing. His son, Case, was found to have a large lung AVM after undergoing HHT-specific screening, which was embolized before any complications arose. Left untreated, large pulmonary AVMs can lead to brain abscess, stroke, and respiratory compromise.
The specialists at IHTC encourage everyone who takes care of patients—including APPs—to watch out for potential signs of HHT. Referring patients with suspected cases for screening can help ensure an early diagnosis for those who have it—and a successful treatment course.
Telangiectasias are malformations of blood vessels that present as small red dots, and are commonly found on the lips, tongue, face and hands. A common sign of HHT is skin and mucosal telangiectasia • Presents as small red/purple pinpoint spots with numbers increasing with age • May not be visible or easily identified until someone has reached their thirties or forties |
“hereditary-hemorrhagic-telangiectasia-62558.jpg”. Copyright © 2019 OMICS International – Open Access Publisher. Reproduced under Creative Commons Attribution 4.0 International (CC BY 4.0). Accessed May 6, 2019 at: https://www.omicsonline.org/italy/hereditary-hemorrhagic-telangiectasia-peerreviewed-pdf-ppt-articles/. |
Dr. Magdalena Lewandowska is an adult hematologist at the Indiana Hemophilia & Thrombosis Center (IHTC) in Indianapolis. Dr. Lewandowska leads IHTC’s HHT Clinic, as well as the center’s Girls & Women Only (GO) Clinic—Indiana’s only dedicated clinic for adolescent girls and adult women with bleeding or clotting disorders.